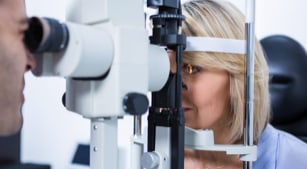
Certain factors play a role in how quickly glaucoma can lead to vision loss. Glaucoma is a serious eye condition characterized by a damaged optic nerve. Glaucoma causes the person to lose patches of their peripheral vision.
Glaucoma is the second leading cause of blindness in Canada. More than 250,000 Canadians have chronic open-angle glaucoma, which accounts for 90% of all glaucoma cases.
Since glaucoma is a slowly progressive neurodegenerative optic nerve disease, early detection and treatment can significantly protect against a potential loss of vision.
What Causes Vision Loss in Glaucoma
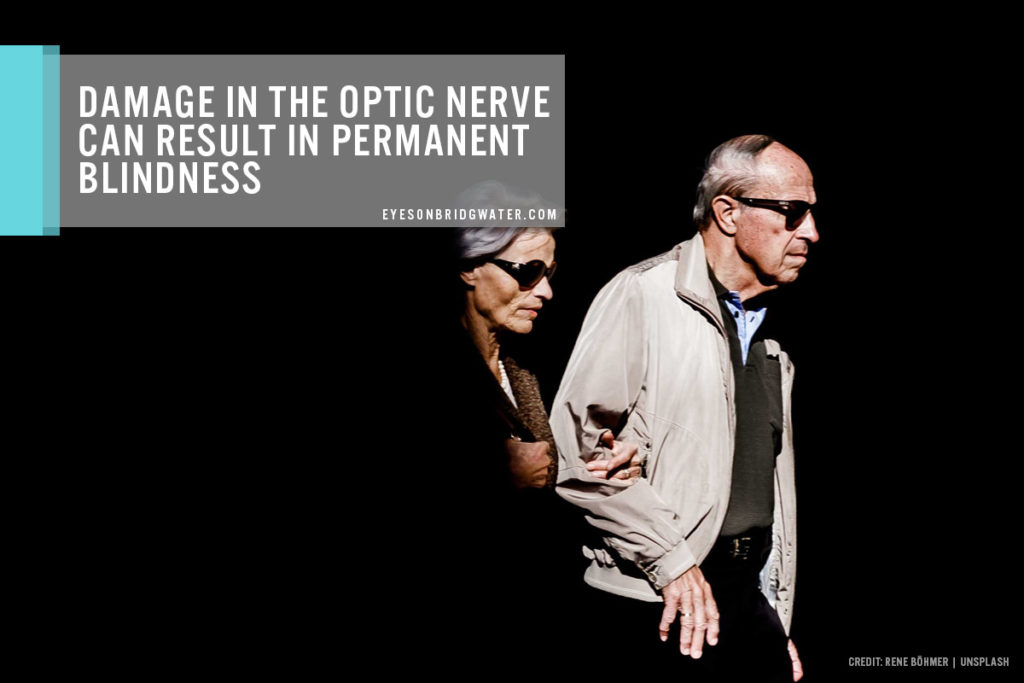
The causes of glaucoma remain unclear. However, glaucoma damages the optic nerve, causing increased pressure in the eye, also known as intraocular pressure (IOP). This is an important factor most doctors look into. Healthy eyes naturally produce aqueous humour, a watery fluid that flows through the pupil and behind the clear cornea and drains through the trabecular meshwork.
When the eye cannot drain the fluid properly, pressure starts to build inside the eye, damaging the optic nerve over time. This eventually causes the optic nerve fibres to die. However, in some cases, the optic nerve can still become damaged even without increased pressure. Some eye health experts claimed that some glaucoma patients may be unusually sensitive even to normal eye pressure levels while others believe that eye blood flow problems may be a contributing factor.
Glaucoma of the eyes affects people differently. In most cases, glaucoma initially affects the peripheral vision of a person. Over time, late-stage glaucoma may experience tunnel vision, where the affected person can only see straight ahead. Untreated glaucoma could result in total vision.
Understanding the Types and Symptoms

Glaucoma comes in different forms. Often, knowing the cause of high pressure in the eye helps eye doctors determine the type of glaucoma and the right treatment for the disease.
Below are the most common types and symptoms of glaucoma that are classified into primary and secondary:
Primary Glaucoma
- Open-Angle Glaucoma
Open-angle glaucoma is the most common type of glaucoma, which accounts for 90% of all cases in Canada. Too much pressure in the eye (IOP) causes damage to the optic nerves due to inefficient drainage of the aqueous fluid. IOP causes significant optic nerve damage by reducing blood flow to the nerve. The pressure building up within the eye can also squash the nerve. Some people can have open-angle glaucoma even without elevated eye pressure.
Symptoms:
POAG in its early stage does not have any apparent symptoms. A person with early-stage POAG is not aware of the damage until the condition progresses and becomes permanent. The symptoms usually go undetected because the damage takes place in the off-centre parts of the field of vision. Since both eyes work together by filling in for each other, blank patches often go unnoticed.
- Primary Acute Closed-Angle Glaucoma
When the iris comes forward, it closes the drainage angle, blocking the eye drainage system and increasing the eye pressure due to fluid buildup. Unlike the primary open-angle glaucoma, this type of glaucoma can happen in an instant and requires immediate medical attention. If left untreated, it could result in blindness in one eye.
Immediate treatment helps recover vision completely.
Symptoms:
Primary symptoms include:
- Severe eye pain
- Red eyes
- Cloudy vision
- Seeing halos around the light sources
In some cases, sub-acute attacks usually occur in the evening. Common symptoms of sub-acute attacks include:
- Misty vision with coloured rings around white lights
- Eye redness
- Discomfort
- Secondary Glaucoma
This type of glaucoma is caused by the narrowing of the natural drainage angle. When the iris presses against the trabecular meshwork, it causes significant damage or closes the drainage angle. IOP is usually higher in secondary glaucoma due to damaged trabecular meshwork.
Symptoms:
Common symptoms of secondary glaucoma include: eye pain with cloudy vision
Early-stage glaucoma shows no symptoms — vision is perfectly normal and there is no pain. However, when glaucoma progresses in its late stage, a considerable amount of the field of vision is lost. People with late-stage glaucoma may find getting about and using stairs difficult.
- Developmental (Congenital) Glaucoma
This type of glaucoma is common in infants and children. When the normal eye filter is not fully developed, it prevents the normal drainage of aqueous fluid, causing the eye pressure to rise. Development glaucoma may run in the family.
Symptoms:
Common symptoms of developmental (congenital glaucoma) include:
- Enlarged eyes
- Sensitivity to light
- Cloudy and watery eyes
- Poor vision
- Jerky eyes.
Reducing Your Risk of Glaucoma-Induced Blindness
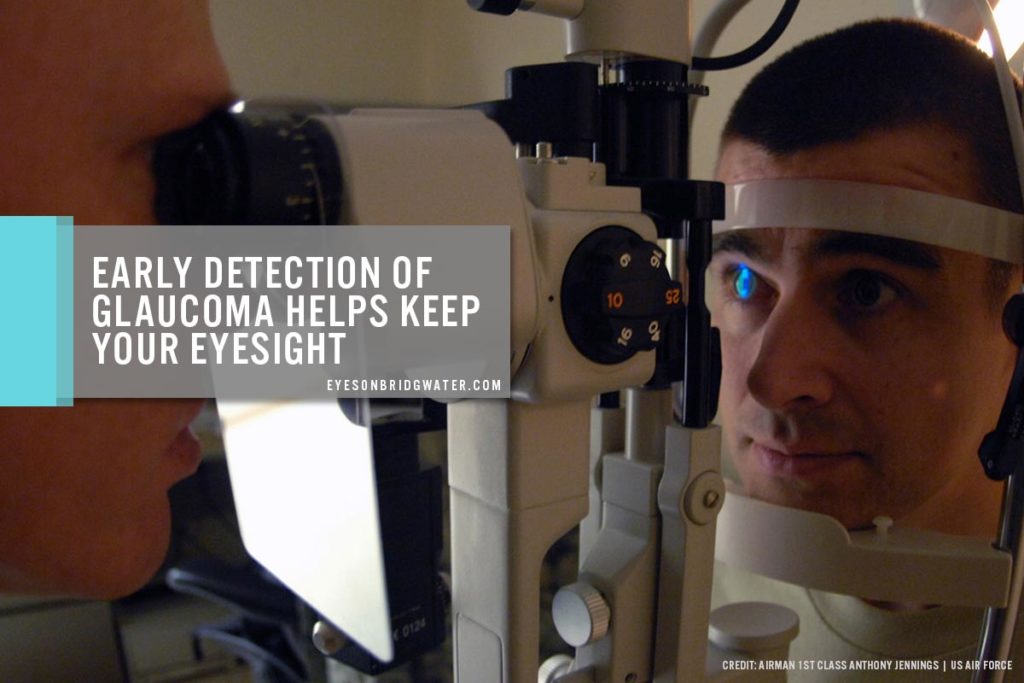
Although most people do not experience any symptoms, having your eyes checked regularly can help confirm glaucoma signs using state-of-the-art eye exam equipment. If you experience any problems in your vision, do not hesitate to visit your trusted eye doctor and get a blindness test as soon as possible to prevent long-term loss of vision.
The loss of vision cannot be restored, but reducing eye pressure helps you keep your sight; that is why eye health professionals recommend glaucoma patients to undergo a regular glaucoma test and follow their treatment plan.
Here are some of the eye exams conducted to detect glaucoma:
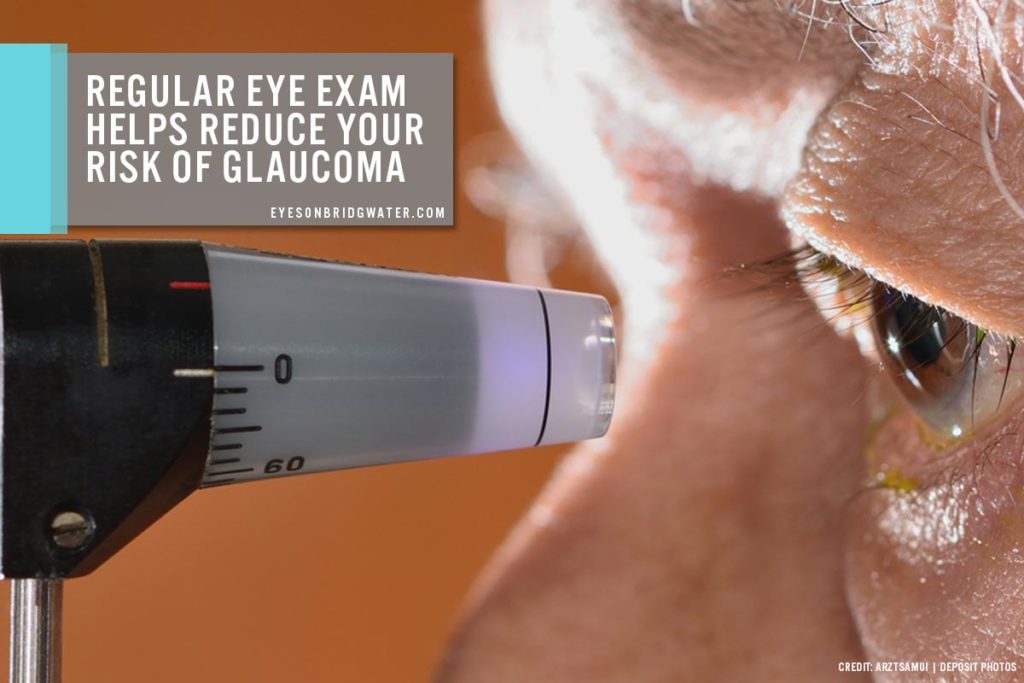
- Eye Pressure Check
Increased eye pressure is an important vital sign to look into when visiting your eye doctor. Eye pressure test (tonometry) is a quick and painless method that measures eye pressure.
During the test, eye drops are used to numb the eye and a tonometer is used to measure the eye’s inner pressure. The eye doctor applies a small amount of pressure to the eye using a small device or a warm puff of air. The normal eye pressure range is between 12 to 22mm Hg, but in most glaucoma cases, the pressure exceeds 20mm Hg.
- Visual Field Test
Considered a function test, the visual field test enables the eye doctor to detect any signs of visual field loss due to glaucoma and determine the rate of disease progression, helping them to create a personalized treatment for the patient.
The test is painless and only takes a couple of minutes to examine each eye. It does not require any special preparation and the removal of contact lenses during the test is not needed.
- Glaucoma Imaging Test
The glaucoma imaging test is non-invasive and does not involve the use of radiation. Most eye doctors use it to monitor glaucoma progression.
During the test, the doctor uses eye drops to dilate the pupil and take a photograph of your optic nerve with a digital camera or other technologies to map the optic nerve. The test results are immediately available and will be projected on a computer screen.
- Dilated Eye Exam
During the dilated eye exam, the ophthalmologist will assess your glaucoma by dilating the eyes to obtain a magnified, 3D view of your optic nerve to determine the condition of the optic nerves and glaucoma. The current colour, shape, depth, size, and vessels of the optic nerve will be assessed. The dilated eye exam will also include a thorough examination of the central and peripheral retina.
- Cornea Thickness Test
Also known as pachymetry, the cornea thickness test is a painless way to measure the corneal thickness using a small probe after numbing the eye with an eye drop. A thin cornea contributes to low eye pressure reading, while a thick cornea contributes to a higher-than-normal pressure reading. The risk of glaucoma is more prevalent in people with a thin cornea.
- Angle Test
Otherwise known as gonioscopy, the angle test is a simple, quick, and painless procedure that allows the optometrist to examine the angle where the cornea meets the iris. Since the “angle” is where the trabecular meshwork is located, gonioscopy enables the doctors to classify the trabecular meshwork as an “open” angle if it is visible and “closed” angle if the iris or a scar tissue blocks the trabecular meshwork.

If you suspect you have high-risk glaucoma, how to prevent the condition should be a top concern. Make sure to visit a trusted and reliable optometrist at Eyes on Bridgwater for a comprehensive eye exam. Call us at (204) 230-0422 to book an appointment.